- Unless something changes, this story which might have happened forty years ago, will still be happening in forty years time
- Everything seemed well with their second child, their parents helped out and her mother returned to work. But at nine months old, Anna started vomiting, every morning without fail, settling by the afternoon. She was distressed with the sickness, crying constantly. In every other way she developed normally, walking, talking, playing and generally being a toddler.
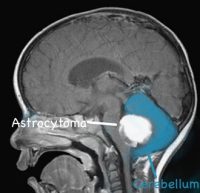
- However she continued to vomit. Over the next nine months, her parents visited numerous doctors, both privately and within the NHS. Diagnoses ranged from tonsillitis, ear infections, stomach infections and the local hospital even said there was nothing to worry about and as Anna was simply “attention seeking”? However she didn’t get better and in one terrifying episode, her eyes all but disappeared, leaving only the whites of her eyes visible “the setting sun” sign. A few days later, her parents again rushed her to hospital because she wouldn’t wake up. She was admitted as an emergency. Finally there was a diagnosis, Anna had a brain tumour at the back of her skull. A pilocytic cerebellar astrocytoma.
- Anna needed urgent surgery. She recovered well from surgery and didn’t need any other treatment. She learnt to walk and talk again, but was left with an odd walk, strange arm movements and poor balance. She was discharged to the care of her General Practitioner, the one who failed to diagnose her tumour. I saw her in part because of the difficulties she was having at school.
HOW IT COULD HAVE BEEN DIFFERENT
There are two parts to this little girl’s story.
1 – The Initial Diagnosis
Anna’s story is sadly typical for a child with a brain tumour, relentless vomiting and headaches, worse in the morning. The “setting sun” sign when the eyes disappear downwards indicates severely raised pressure inside her head as do the headaches and vomiting. In fairness, the vast majority of children who cry and vomit do not have a brain tumour but very occasionally they do.
Everybody in the land needs to be aware of the possibility of a child having a brain tumour. This is a classic story of one such child. I started my medical life as a neurosurgeon and this story was typical of just about every child we saw. It is extremely rare but it happens. Sherlock Holmes: “Once you have eliminated the impossible, then what is left, however improbable must be the truth”
Making Diagnoses is the single most important reason for being a doctor. Unless you know what is causing a problem, you cannot effectively treat it. And if your treatment isn’t working, you need to go back and make sure you have the right Diagnosis. And if the Diagnosis is right and the treatment is not working, you need to carry on trying to work out what is going on, until you have done all you can.
Traditionally a Diagnosis is made through the following steps:
1) See the patient and take their history,
2) Examine the patient
3) Form a list of possible or “differential” Diagnoses and
4) Confirm the correct Diagnosis using the limited investigations at your disposal and following the patient over time. This method began with Hippocrates and Galen, Greek physicians working almost two thousand years ago, long before the rise of reliable technology.
We are living in a different world. Blood tests and scans are cheap and reliable. True medical expertise is now the scarce resource. No one wants to return to the days of making a Diagnosis as the patient walked through the door because their condition was so far gone that it was immediately obvious. Modern disease is subtle, and far harder to spot. It is hard to spot someone with diabetes or who has had a heart attack or mental health problem.
If doctors as Diagnosticians are going to be effective, we have to use technology differently – Technology needs to come first. Blood tests, scans MRI and Ultrasound are cheap and safe. Those investigations that have side effects, such as X-rays should not be freely available, but if the test is safe, then it needs to be freely available “Over the Counter”. Google can answer any questions you may have and the patient then follows up with the doctor.
As doctors we need to give patients credit for knowing what they and their children might need. In the UK, everything goes through the General Practitioner (GP) who, at best, knows a little bit about many things but is not a specialist. GPs decide what needs to be done using Algorithms decided by the National Institute of Clinical Excellence (NICE). These guidelines dictate how medical conditions should be investigated and treated. If GPs can follow an algorithm, without doubt, AI can do so faster and more accurately.
Diagnosis matters, doctors are a scarce resource and they need information at their fingertips even before they see the patient. By putting technology first, before we give an opinion, doctors really can Save Lives. MRI scans are cheap, cheerful and revelatory. AI can do the grunt work of finding out about the patient’s problem and organising initial investigations and then a fully informed the doctor can set to work to see if the problem is serious and what needs to be done next.
2 – Follow Up Assessments – Problems don’t go away
When a developing brain has been damaged by nine months of high pressure, a near death experience, and then major lifesaving surgery, that child is going to have long term problems. These may subtle enough to work around or serious enough to affect her life chances. In order to give that little girl the best chance in life, she needs proper assessment which, despite all her mothers efforts, was not happening.
Given Anna’s story, there are several areas that need to be assessed in detail.
1 – Eyesight. It is unfortunately more likely than not that Anna’s eyes were damaged by prolonged raised pressure inside her head caused by her tumour. Her mother says she does not see things put down in front of her, she bumps into doors and she frequently falls over. She doesn’t have friends, could this be because she doesn’t see the other children properly?
2 – Balance problems. The cerebellum helps movement and balance. The tumour will have directly damaged this part of her brain. A specialised neurologically trained physiotherapist could help Anna improve and maintain her balance.
3 – Anna still wets and soils herself. Why? There is no obvious reason, so it needs to be investigated.
4 – Special Educational Needs (SEN). Anna is on the SEN register. Her school are aware of her problems but are doing very little to help her. Anna cannot read or write, and has to sit near the front of the class. How much of her problems are due to her poor sight or does she also have intellectual impairment that makes it hard for her to understand and learn what she needs to do. Every child is precious, she may not become a great novelist but she still deserves her place in society.
5 – Social integration and bullying. Anna struggles to fit in at school. She looks slightly strange, with her odd walk, arm movements and toilet problems. The school are aware she has problems, but have not stopped her classmates bullying her mercilessly.
6 – In class Anna tends to sit quietly at the front. “Support” in a school already overburdened with poorly performing pupils, is hard to come by.
As far as Anna is concerned, the damage was done before she was two. Nonetheless, the brain can do a lot to repair itself, in the right environment. Remediation needs to be offered early if it is to make a difference. Now she needs help to make the most of those abilities she does have and help developing strategies to allow her do as much as she can. This has to include an up to date MRI scan, a full physical and medical assessment, including eyesight and hearing as well as a full psychological and educational assessment in order to understand her difficulties and the best way to help her at this stage.
There are no short cuts. It is cheaper and more effective to be proactive, not reactive and prevent damage, rather than try and repair it later.
“You cannot manage what you do not measure”